About diabetes
1 in 11 adults are living with diabetes2
Diabetes mellitus is a serious, long-term condition that nearly half a billion people are living with worldwide. It occurs when there are raised levels of glucose in a person’s blood because their body cannot produce any or enough insulin, or cannot effectively use the insulin it produces.
Insulin is an hormone produced in the pancreas that enables glucose from the bloodstream to enter the body’s cells, where it is absorbed and converted into energy. If the body produces insufficient insulin, or the cells are unable to respond to it, the blood glucose levels will rise causing hyperglycemia, which is the clinical indicator of diabetes.

The estimated prevalence of diabetes (Type 1 and Type 2 combined, both diagnosed and undiagnosed) in people aged 20–79 years has risen to 463 million (9.3% of the global population). Without sufficient action to address the pandemic, it is predicted that 578 million people (10.2% of the population) will have diabetes by 2030. That number will jump to a staggering 700 million (10.9%) by 2045.3
Type 1 diabetes is the result of an autoimmune reaction in which the body’s immune system attacks the insulin-producing cells of the pancreas – producing, as a consequence, very little to no insulin. Currently, the cause of this destructive process is not fully understood and cannot be prevented, but is likely to be explained by the combination of genetic susceptibility and an environmental trigger initiating the autoimmune reaction.
Type 1 diabetes can develop at any age, but occurs most frequently in children and young people.
People with Type 1 diabetes need daily insulin injections to maintain a glucose level in the appropriate range. Without it, patients with Type 1 diabetes would not survive. However, with appropriate insulin treatment, regular glycemic control, education and support, they can live healthy lives and prevent or delay many complications associated with diabetes.
Type 2 diabetes is the most common type of diabetes, accounting for around 90% of all diabetes worldwide. In Type 2 diabetes, there is a situation called ‘insulin resistance’ during which the insulin hormone is ineffective and the body’s cells are unable to respond fully to it. As a result, there is an increase in insulin production and hyperglycemia. Currently, the causes of Type 2 diabetes are not fully understood but there is a strong link with overweight and increasing age, as well as with ethnicity and family history. It results from a combination of multi-gene predisposition and environmental triggers.
Type 2 diabetes is more common in older adults, but it is increasingly seen in children and younger people due to rising levels of obesity, physical inactivity and inappropriate diet. The cornerstone of Type 2 diabetes treatment is the promotion of a healthy lifestyle, including increased physical activity and a healthy diet. However, if attempts to change lifestyle are not enough, oral medication (or insulin) will be required to control blood glucose levels.
- Gestational diabetes develops sometimes during pregnancy but usually disappears afterwards.
- Other rarer types of diabetes also exist.
Over the long term, high glucose levels are associated with the development of serious and life-threatening complications and the reduction of quality of life.
Consistently high blood glucose levels can lead to damage of many of the body’s organs, leading to disabling and life-threatening health complications such as cardiovascular diseases, nerve damage (neuropathy), kidney damage (nephropathy), eye disease (leading to retinopathy, visual loss and even blindness) and diabetic foot complications (leading to lower limb amputation).
About DIABETIC FOOT COMPLICATIONS
Diabetic foot is one of the most common,
costly and severe complications of diabetes.
There are several factors that lead to diabetic foot
ulceration and low likelihood of ulcer healing:

Loss of Protective Sensation (LOPS)
Diabetes is associated with LOPS due to Neuropathy. Neuropathy is the damage of the nerves due to chronic high blood glucose. When peripheral neuropathy appears (which is the most common form of diabetic neuropathy), nerves lose their effectiveness: whether it is their motor, sensitive or autonomic functions.
Loss of Protective Sensation (LOPS) makes the foot susceptible to trauma, as it allows injuries to go unnoticed, leading to ulceration. Patients with LOPS can lose their normal ability to perceive pain, heat or cold on their feet. When proprioception is reduced, patients become unaware of position of their foot when walking, which can cause significant stresses on their bones and joints. As a result, the foot can respond by growing hard skin (callus), which may lead to foot deformations and ulceration.
For instance, patients with LOPS can cut themselves on the foot when stepping on glass without noticing it.

Foot deformities
For a diabetic, foot complications are an ever-present risk. This risk further increases if you have foot deformities. For people living with diabetes, damage to the nerve supply of foot muscles causes weakening of the muscles and a change in shape of the feet. This creates abnormal pressure points and bony prominences which can cause sores and ulceration.
The most common foot deformities in diabetes are: hammer toe, claw toe, hallux valgus…
Peripheral arterial disease (PAD)
PAD is promoted by smoking, high blood pressure and hypercholesterolemia.
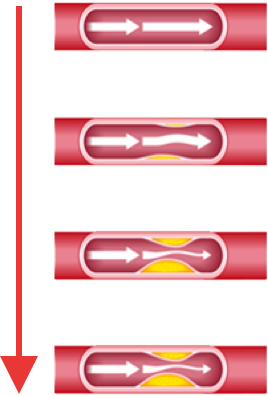
Diabetes promotes the deposition of cholesterol on the walls of the arteries of the lower limbs, and contributes to the formation of atheroma plaque. As a result, blood flows through the legs and feet with difficulty as the arteries in the legs become narrowed or blocked (arteriosclerosis). If the supply of blood to the tissues of the foot becomes poor, the foot becomes more susceptible to injury.
Because of that, PAD increases the risk of foot ulceration and their severity.
PAD may affect the delivery of oxygen in the muscles (ischaemia), which can cause leg pain and the so-called ischemic ulcers. These are very painful arterial ulcers that can affect the leg, the edge of the foot or the ends of the toes, or appear as necrosis.
In case of neuropathic or traumatic injury, PAD will aggravate the situation because of the reduction of oxygenation – and healing may be delayed or even impossible.
When an artery is blocked or narrowed, the part of the body it supplies doesn’t get enough oxygen. The condition is called ischaemia.
Previous history of foot ulceration or amputation
After successful healing, the recurrence rates of diabetic foot ulcers are 40% within a year and 65% within 3 years.4
“Thus, it may be more useful to think of patients who have achieved wound closure as being in remission rather than being healed”
TYPES OF DIABETIC FOOT
There are 3 different types of diabetic foot ulcers depending on the presence of neuropathy (LOPS) and ischaemia (PAD)
Neuropathic diabetic foot ulcer

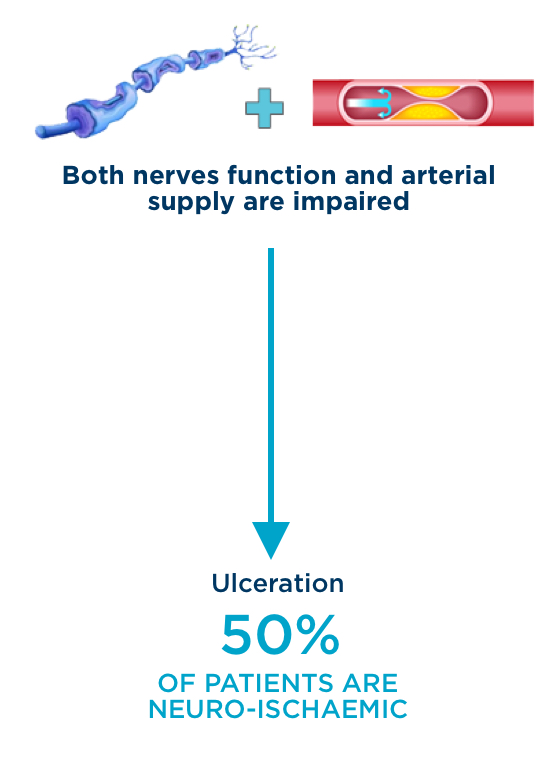
Neuro-ischaemic diabetic foot ulcer
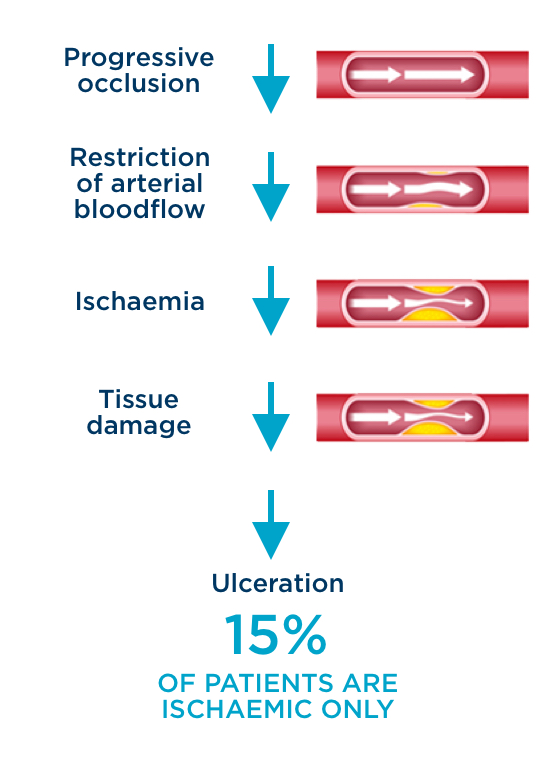
Ischaemic diabetic foot ulcer
Neuropathic foot ulcer
- Etiology: damaged nerves
- Wound bed: pink and granulating
- Location: weight bearing areas (metatarsal heads, heel, over the dorsum – claw toes)
- Sensory loss
- Callus present and often thick
- Dry skin and fissuring (cracks)
- Hyperkeratosis
- Foot deformities
- Foot warm with bounding pulses
Ischaemic foot ulcer
- Etiology: restriction of arterial blood flow
- Painful
- Necrosis common
- Foot cold without pulses
- Wound bed: pale and sloughy with poor granulation tissue
- Location: tips of toes, nail edges, between the toes and lateral borders of the foot
Neuro-Ischaemic foot ulcer
- Etiology: both nerves function and arterial supply
- Degree of sensory loss
- Variable callus
- Prone to necrosis
- Foot cold without pulses (potentially)
- Wound bed: poor granulation tissue
- High risk of infection
- Location: margins of the foot and toes, everywhere on the foot
the consequences of diabetic foot

1 in 4
people1
 1 in 4
1 in 4people1

every 20
seconds5
 every 20
every 20 seconds5

70% of amputated
patients3
 70% of amputated
70% of amputatedpatients3
A DIABETIC FOOT CAN BE LIFE-THREATENING
Due to diabetic foot, people with diabetes are 15 times more likely to undergo amputation than other people.
Diabetes has become the leading cause of amputations worldwide. The lives of people after an amputation are profoundly affected: many are unable to work, become dependent upon others and cannot pursue an active social life. Physical, emotional and social functions are all affected and depression is a common occurrence.
Five years after a lower extremity amputation, up to 70% of people may have died.
IN THEIR OWN WORDS
Discover real testimonials of patients with history of diabetic foot.
1. Setacci C, de Donato G, Setacci F, Chisci E. Diabetic patients: epidemiology and global impact. J Cardiovasc Surg (Torino). 2009 Jul, 50(3) : 263-73
2. International Diabetes Federation Atlas – 9th edition 2019
3. Saeedi P. et al. Global and regional diabetes prevalence estimates for 2019 and projections for 2030 and 2045: Results from the International Diabetes Federation Diabetes Atlas, 9th edition. Diabetes Research and Clinical Practice 157 (2019) 107843
4. Armstrong DG, Boulton AJM, Bus SA. Diabetic Foot Ulcers and Their Recurrence. N Engl J Med 2017; 376: 2367–75.
5. Whiting, D. R., Guariguata, L., Weil, C., and Shaw, J. 2011. “IDF Diabetes Atlas: Global Estimates of the Prevalence of Diabetes for 2011 and 2030.” Diabetes Res. Clin. Pract. 94 (3): 311-21.
Fortunately, clinical studies have shown that foot ulcers can be prevented and successfully treated through more prevention, early identifications of patients at higher risk for foot ulceration and appropriate referral of patients presenting with a diabetic foot ulcer to specialised settings.



